A year ago, Vicki and I met a brilliant gentleman, Dr Daniel J. McCloskey, who is Deputy Director of the Clinical Transplantation Laboratory at The Royal London Hospital.
Daniel McCloskey is a tissue typing veteran of some 30 years and he was kind enough to spare us his time to help unravel some of the mystique and answer some of the many questions we had back then.
We remained in touch and have recently had various fascinating chats about what he referred to as ‘the generation of mixed cultures and genes’.
As Daniel explains:

It’s not obvious: Delete Blood Cancer UK are running a “What are you made of?” campaign. Click Margot’s image above to find out more
“Simplistically, our tissue type is a series of genes, inherited from our parents, which make important proteins crucial for us to have a good immune system to combat bacteria, viruses and other diseases (pathogens). Our immune system is very good at recognising pathogens (non-self) and differentiating it from us (self) and making an immune response to pathogens to get rid of them.
Some patients with blood cancer or gene defects of the immune system need a new immune system which they can get by what is commonly called a bone marrow transplant. This is the transplantation of immune cells from the donor to the patient which can be bone marrow or special cells isolated from the blood of the donor (peripheral blood haematopoietic stem cells). The transplant process is the transfusion of donor cells into the patient.
Traditionally the patient and donor are matched for up to 10 antigens of their tissue type. For a bone marrow transplant patient, the ideal scenario is where a “perfect” 10/10 donor match can be found. The donor cells can be transfused into the patient without too many complications arising. The major complication which may arise is when the donor cells recognise the host (patient) cells as foreign (non-self) and so they attack the host cells. This is called “graft versus host disease” or GVHD for short. When a fully matched donor is not available, successful transplants can be performed with mismatched donors but the possibility of GvHD is increased.
Donors can be related like siblings who have a 1:4 or 25% chance of being a tissue type match. For patients with no matched family donor, an unrelated donor needs to be identified through one of the many Stem Cell registries around the world. However, the registries are not evenly distributed around the world and many ethnic groups are under represented.
Over hundreds of thousands of years the tissue types of different populations have evolved to combat the diseases in the environments where those populations live. Consequently tissue types and their frequencies do vary between different populations and the best chance of finding an unrelated donor is in the population of ethnic group of the patient.
However an added complication over the last century, with long distance travel and migration becoming commonplace together with changes to cultural barriers, there is an increase in mixed race relationships on a scale never seen before. Consequently there is an increase in children who become the next generation that are mixed race genetically.”
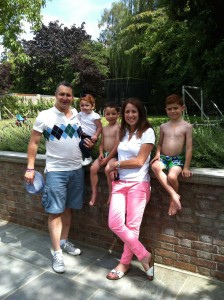
This is what we looked like: the day we left to take Margot to Sheffield for some experimental treatment in July 2014. We had been told that Margot was ‘conventionally incurable’ at the time, after both leukaemic clones relapsed
In our family, Vicki & I only have to look as far as our own parents for first hand examples of this social change in action: Vicki’s parents are from New Zealand and England respectively, whilst mine are a mix of Scottish, Siamese (Thai) and Syrian, with a dash of Armenian.
So it stands to reason that Margot was mixed race – born from a generation of mixed cultures and genes. And rather an unusual mix at that.
This helps to explain why it shouldn’t be too great a surprise that we were unable to find Margot her perfect donor match, although we were fortunate enough to find a 9/10 donor match, which the doctors referred to as being a “suitable match”.
Margot’s experience underscores how hard it can be to find matches for people with mixed heritage. And moreover, taking into account Daniel’s comments: “the ethnic minorities of today are one thing, but the ethnic minorities with additional mixed races are increasingly tomorrow’s problem.”
The practical reality is that this issue is likely to become ever more problematic. Our children’s children are the donors of the future and they will also be the generation of patients with the biggest problems to date in finding donor matches.
This is why Team Margot encourages not only the recruitment of donors from the ethnic minority groups but also those with a mixed heritage to join the worldwide stem cell registries.
The more this happens, the more lives will be saved.
Thank you for the wonderous insight Daniel and for being fantastically supportive to our family & Team Margot !
Team Margot
Together, saving lives
Husband to Vicki and father to Oscar (2007), Rufus (2008), Digby (2015), Humphrey (2017) & Margot (2012-2014)
Team Margot’s mission
To help save and improve lives by educating, inspiring and motivating people, especially from ethnically diverse communities, to register as blood, organ and stem cell donors.