I have been looking back at the private blog that I began keeping a few days after Margot was first diagnosed with leukaemia. Only a year has passed and yet I’m surprised at how much I actually remember or more particularly, how much I have already forgotten ! and so I thought I would share some thoughts on what was happening around this time last year, not least because it helps provide a little more background and insight into the donor search process.
25 November 2013 was a milestone day, being 50 days post diagnosis, and at the time we felt that we were in a relatively good place, all things considered.
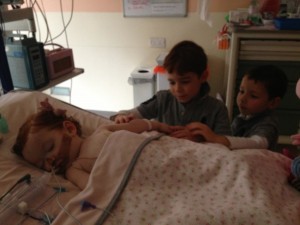
Margot’s brothers, Oscar & Rufus visit her in PICU
On 7 October 2013 Margot had been diagnosed with an extremely rare form of leukaemia and she required an immediate exchange transfusion (new blood) and intensive chemotherapy treatment on arrival at Great Ormond Street Hospital (GOSH). Margot was on life support and in an induced coma in the Paediatric Intensive Care Unit (PICU) for most of her first 10 days in hospital and had since made a slow but steady recovery, making small progressive steps each day.
The overriding goal was of course to try and eradicate the leukaemia and then reboot Margot’s “blood factory”; the plan was to deploy three courses of chemotherapy to bring the leukaemia into temporary remission and then follow up with a bone marrow transplant.
Margot had been given an A+ by the doctors for the way in which she had responded to her first month of chemotherapy. Her second course of chemotherapy had begun as soon as she was well enough, following a brief respite at home. Again, so far, Margot was responding to this latest bout of chemotherapy as well as could be expected. It was a much more intensive dose than the first and administered over a shorter 5 day period only. Our hope was that Margot would recover from this second phase of chemotherapy by the third week of December, in time for another short break over Christmas.
The doctors continued to steer us towards Margot having a bone marrow transplant, because it offered her the best chances of beating her blood cancer once and for all. However, before a transplant could be embarked upon, we first needed to identify a matching bone marrow donor for Margot.
At the time, we had already established that we didn’t have a donor match for Margot within our immediate family and therefore an official search for a suitable donor had begun. This search was undertaken by the transplant team at GOSH and is typically a 10-12 week process. Our most recent information on this ongoing search had been on 8 November (some two weeks prior), at which point we were told that the team were “confident” that a suitable match for Margot would be found & that it was “almost certain” they would find a 9/10 HLA (Human Leukocyte Antigens) match for Margot. During early November a number of likely donor candidates had been identified, including three people in Brazil with a 6/6 antigen match. It all seemed to be going in the right direction, but more of that later…
By way of brief explanation: our tissue type is made up of 10 antigens, so a perfect scenario is when all 10 antigens of the donor and recipient match. That’s the ideal: a 10/10 match, also know as a “perfect match”. If a perfect match cannot be found, then the bone marrow transplant team will consider an unrelated 9/10 or perhaps even an 8/10 match as suitable, but in each case the risk of “graft v host” disease (GVHD) increases. And GVHD can cause serious life threatening complications.
The practical reality is that in many instances, the various databases that exist around the world only record 6 of the 10 antigens. So in the case of the potential three Brazilian donors that were in our line of sight, the process was to then seek to contact the potential donors & ask them to come into their local centre for a blood test to re-check their tissue type and specifically the unrecorded 4 antigens.
Only then could we hope to compare like with like & establish the chances of finding Margot a 9/10 or better match.
This very manual process is the main reason why an international donor search can take so long. Often, one of the biggest challenges is physically finding the potential donor, who may have changed their contact details or moved home since joining the stem cell register.
Our concern with all of this was the absence of any certainty; whilst it was lovely to see Margot responding to the initial treatment as well as she had, we knew the underlying reality of our situation was that we were left waiting and without an identified and confirmed donor, we really didn’t have any visibility as to Margot’s longer term prognosis.
I wrote: ‘as of Friday 21st November 2013″there have been no further developments with the donor process to report”, so we continue to be thankful for the progress Margot is making and to live in hope.’

A year ago – Margot during ‘count recovery’: monitoring blood results post chemotherapy. Simultaneously, an official search for a donor match for Margot was underway.
Husband to Vicki and father to Oscar (2007), Rufus (2008), Digby (2015), Humphrey (2017) & Margot (2012-2014)
Team Margot’s mission
To help save and improve lives by educating, inspiring and motivating people, especially from ethnically diverse communities, to register as blood, organ and stem cell donors.